|
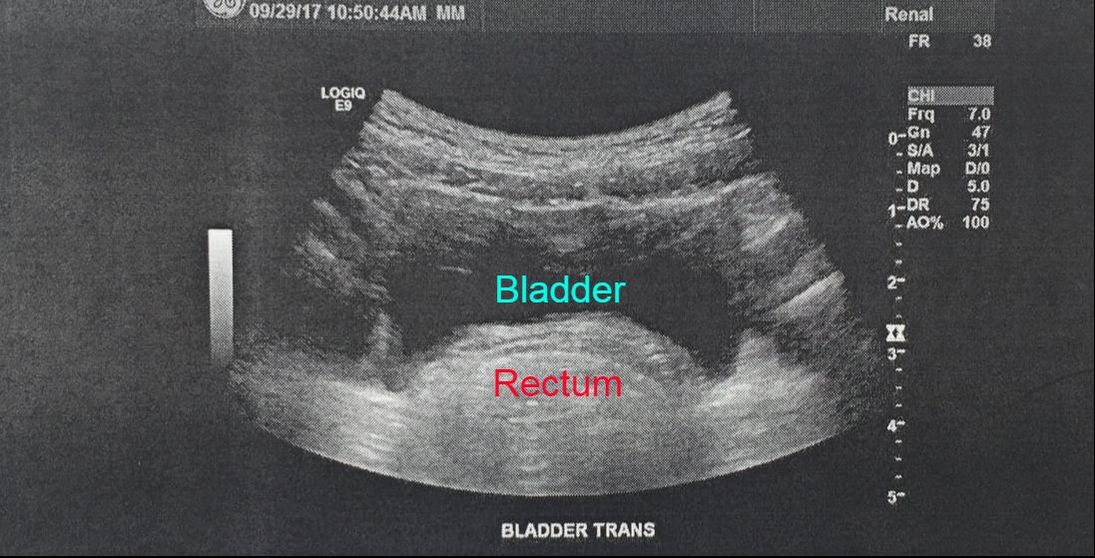
Sorry for the delay in writing updates! We've had a lot of appointments the past few weeks, and I've finally had a chance to sit down and write. I'll try to keep it is a brief as possible without leaving out important information. I also want to warn you that some of the updates involve information about constipation and how the digestive system works. Sorry if it makes any squeamish, but for those reading the blog looking for information related to their own health, those details are pertinent. So on October 2nd, the day finally arrived when one of our daughters had the opportunity to meet and be evaluated by the geneticist that specializes in Ehlers-Danlos Syndrome (EDS). Our oldest two daughters have been on the wait list to see him since March 2016, which puts us at 19 months of waiting. We were expecting to wait for 2 years and were so relieved when her GI motility specialist reached out to the geneticist and got her appointment scheduled so quickly. Yet, now that the day was finally here, I was a nervous wreck. So much has been hinging on this appointment, and so many of the girls' other doctors and specialists have been waiting for this evaluation too. As I was driving the 90 minutes to get to the appointment, all I could think of was how much I hoped he would provide help, answers, and confirmation that our 5-year-old daughter, A, also has Ehlers-Danlos Syndrome. So you can imagine my surprise when, after taking a full medical history on myself and all three of my daughters, the geneticist says, "Well, I wish I was comfortable saying that this was only EDS and that I could fully manage your family's care, but unfortunately I don't feel comfortable saying that at this time." He believes that there may be a bigger diagnosis that would encompass the constellation of symptoms and disorders that the 3 girls have. He's wondering if there is a neurological condition or possibly a mitochondrial disorder, as hypermobility can be caused by other syndromes and disorders. Yikes! That completely caught me off guard. I was expecting this appointment to be either a slam dunk, or like many other appointments, to be let down, dismissed or sent back to the drawing board. Sometimes, when doctors don't have the answers, they send you on your way without any direction or feedback. I've left those appointments feeling defeated, confused and in tears. So I was completely surprised when this appointment took a turn the other way, and he suggested that there is more going on medically that we originally thought. However, when discussing my medical history and symptoms, the geneticist said that it sounded like I have a typical case of EDS. How can that be, but the girls have more? On one hand, I was pleased that he was listening and validated our concerns. On the other hand, I was scared. The fear of the unknown is worse than the fear of the known, at least for me. Or as they say, "Better the devil you know, than the devil you don't know." I guess time will tell, and my questions will have to be answered in about 8 weeks time when we get the genetic test results. He said he would be happy to see our other girls if needed, but that we should wait until the results come back to determine the best treatment plan for our family. In other news, we had a few other appointments over past couple weeks. Our 8-year-old daughter, E, and our 4-year-old daughter, C, were at the hospital to have their clinic appointments with the GI, allergist and nutritionist on October 6th. It's nice to be able to have 6 appointments scheduled together and for the doctors to be able to collaborate. Yet, it also makes for a really long day, leaving the house at 8:00 am and returning by 2:30 pm. So the highlights from those appointments include that both girls continue to be constipated and in need of a bowel clean out. So for 3 days total that weekend, we completed clean outs for all 3 girls, which is never a pleasant experience and requires us to be home bound and missing out/cancelling a lot of activities. The GI added senna to C's medications for the next 2 weeks in hopes of keeping her digestive system moving. We also discussed with the GI and allergist how much C has been coughing, both when running or exerting herself and when drinking fluids. So the GI ordered a video flouroscopic swallow study to rule out aspiration when drinking and the allergist prescribed a rescue inhaler, Albuterol, to use as needed when she has trouble breathing and coughing when exercising or before exerting herself. Additionally, we were advised to stop the peanut butter trial for C for now, since it was causing abdominal pain. We will retest her food allergies in the winter when she is able to stop taking her antihistamines for 5 days prior to the skin allergy test. At that time, we hope to be able to trial foods that were previously triggers and that she is hopefully outgrowing. Then on October 11th, we had 2 important follow-up appointments with the motility specialist and the urologist. This was another very long day as we left the house at 8:45 am to drop off the girls at school, drove to the far north suburbs for the motility specialist appointment, got home around 3:00 pm, picked up the girls from the babysitter and school, had ABA therapy, ate a quick dinner, and then left for the urology appointment at 5:45 pm to get there in time for the 6:40 pm appointment. We didn't arrive back home until 8:00 pm. While these appointments are very important, the days are long and exhausting for all those involved. It also requires asking friends for help with getting kids to and from school, hiring a babysitter to pick up our preschooler and care for her, and for my husband to come home early from work to take over ABA therapy session, help them with homework, and finish the nightly routines before bedtime. I'm grateful for everyone's help, but wish our days weren't so complicated. I long for a simpler life... maybe someday. So first was the follow-up appointment with the motility specialist to go over the 3 motility tests that A, our 5-year-old, had done over the past month, which included the SITZ marker study, the water soluble contrast enema, and the Anorectal manometry test. The SITZ marker study showed that all the markers had been passed, but that there was still a lot of stool in her colon. Thankfully, the contrast enema test was also normal. So that means that her colon is not stretched out, which is surprising but also great news. Finally, the anorectal manometry test revealed that the muscle control in her rectum is abnormal and that she is contracting those muscles instead of relaxing them during an attempted bowel movement. This is likely due to her long history of severe constipation and pain. Her body has adapted to the pain and discomfort. So the recommended treatment is pelvic floor biofeedback therapy to address the pelvic floor dyssynergia. Furthermore, he increased her senna dosage and referred her to the multi-disciplinary bowel management program at the local children's hospital. This team includes the GI motility specialist, a pediatric surgeon, a social worker or psychologist and a nutritionist. That evening, our 4-year-old daughter, C, had her follow-up appointment with the urologist to review the results from the abdominal x-ray, abdominal ultrasound and the spinal MRI. Prior to this appointment, we had received a call from the neurosurgeon that the brain MRI showed a stable pineal cyst (see the post called My 12-hour adventure with "C" for more information), that the spinal MRI was normal, and no tethered spinal cord was noted. While this sounds like good news, it means further evaluation to identify why she's having current symptoms. However, the urologist did share this ultrasound photo with me, which shows C's bladder. He pointed out how her rectum is so full of stool that it is pushing into her bladder in an extreme way. He actually said to me that looking at that photo made him feel like he had to urinate (insert humor), but that in all seriousness, that it looks extremely uncomfortable. It was technically an obstruction and was blocking the elimination of stool and air in her entire colon. So that definitely explains why she has such severe abdominal pain on a weekly, sometimes daily, basis. He recommended that she continue the senna her GI prescribed for the next 3 months to keep her digestive system moving and cleaned out. Hopefully, the bladder symptoms will improve. We follow up with the urologist in 3 months, and she how she's doing. Thank you all for reading and for your support! Please feel free to leave comments or questions below, or contact me directly. It's always nice to hear from you!
Deb
10/17/2017 11:36:57 am
Bekki,
Dianne Guest
10/17/2017 04:11:37 pm
Love and prayers 🙏
Caitlin
10/17/2017 04:15:55 pm
I can only imagine how exhausted you all must be. Thank you for the updates and we are always praying that things improve especially given all that the girls have gone through so far. Love and hugs Comments are closed.
|
AuthorHi, I'm Rebekah! I'm a wife, architect, teacher and mother to 3 amazing daughters! Thanks for stopping by my blog, RAISING ZEBRAS! Archives
February 2018
Categories |