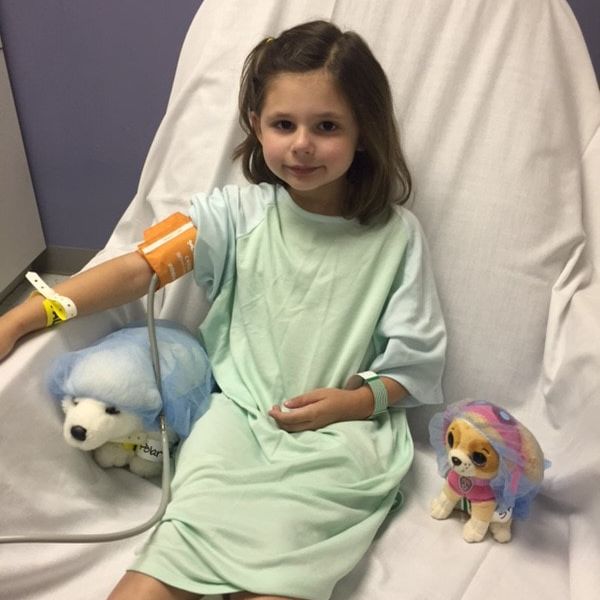
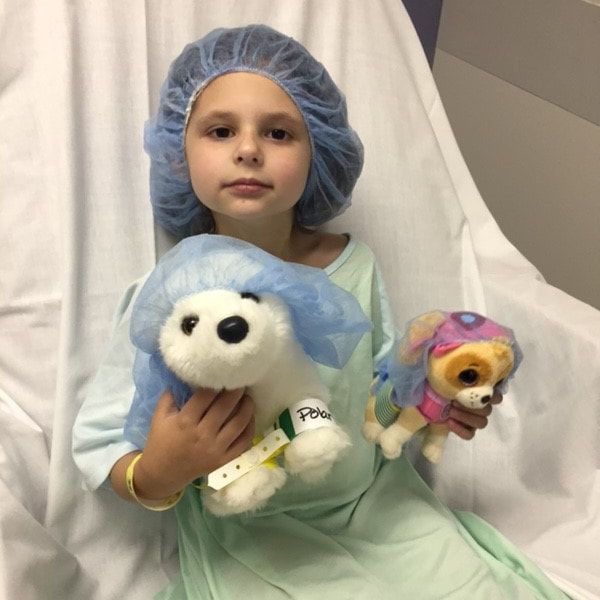
 All ready for her sleep study! All ready for her sleep study! Update Part 1: "Well, you earn the award of The Most Unique Patient of the Day!" These were the words uttered by my doctor last week, and it wasn't the first time I have heard that. Unfortunately, the same message has been repeated several times over the past 8 years, and is common for many zebras to hear over and over again. I heard a similar message on November 22nd, the day before Thanksgiving, at our follow-up appointment with the sleep specialist for our 5-year-old daughter. She completed a sleep study a few weeks ago and we were meeting to go over the results and treatment plan. Unfortunately, A's sleep issues have not improved since her turbinate reduction surgery in September. She is still just as tired throughout the day, falling asleep at all times of the day, and is unable to function properly without a daytime nap. So I approached this appointment knowing that something had to be done to help her and was expecting the recommendation for a CPAP machine. However, the results of the sleep study showed that her obstructive sleep apnea had improved a bit and was now only considered "mild." However, she had an increase in the frequency of periodic and isolated limb movements, which can cause her to be aroused out of REM sleep each time. Despite that disorder worsening, the sleep doctor did not feel that the mild sleep apnea and limb movement disorders were bad enough for her to recommend the CPAP machine or that they fully explained the severity of her hypersomnia. This is what led her to say that A's health struggles are tricky, unique and a bit puzzling. After asking me many questions, going over her medical chart and previous tests again and again, she believes that A is becoming so fatigued from a combination of a possible neurological condition, the mental overload she experiences during a full-day of kindergarten, and her low muscle tone paired with all the physical activity at school. (Individuals on the autism spectrum and who have anxiety, like A, often become very overwhelmed in school environments, which can be very exhausting mentally.) The doctor is hoping the genetic testing we are waiting for will shed some light on the situation and provide some more answers. For now, the doctor's recommendations are to get a second opinion from another sleep specialist at the local children's hospital since A's case is so complex, repeat the sleep study in 6-9 months, have a full neuropsychological evaluation to determine her neurocognitive functions and to help with school accommodations, repeat her blood work to check levels that could be affecting the period limb movements (last time the blood work was all normal), and to consider other ways to incorporate power naps at school, or to reduce her school work load and school hours to half-days. I passed this information on to her school team, and luckily, we meet on Thursday to discuss her current re-evaluation of her IEP (individualized education plan). So together we will come up with a plan that best meets her health and educational needs. Needless to say, this potential schedule change will cause a bit of a shake up in our family. So I'm scrambling to figure out how to make all these changes and quick! I'll be sure to keep everyone updated, of course! Update Part 2: On November 24th, the day after Thanksgiving, our 8-year-old daughter, E, and I had to report to the hospital to complete autonomic testing and be evaluated by the same autonomic neurologist that I see regularly. We were so fortunate to get an appointment in just 3 weeks from calling for these tests. Most patients wait 6-8 months to see him. Thankfully, he knew a lot about E already and had said he recommended testing her to see if her bladder and GI issues were due to autonomic dysfunction and could possibly explain why her incontinence issues have not improved after her tethered spinal cord release surgeries. So when I contacted him about her recent struggles in PE class at school, he thought it warranted a quick evaluation. See, E has been struggling most Thursdays during PE class when they often run longer distances. She has symptoms afterwards each day that include headaches, dizziness, chest pains, and sometimes her pulse ox reading is too low. Each Thursday this year, she ends up in the nurse's office and I get a phone call with an update. Several weeks ago, she started sitting out at PE time when the class was required to run, which she is allowed to do with her current health issues and 504 plan at school, and it gave us the time to schedule the necessary doctor appointments to investigate what was going on. So on the day of testing, E underwent 4 autonomic tests, including sweat testing using a capsule applied to the skin, a measurement of heart rate after deep breathing while lying down on her back, a measurement of heart rate and blood pressure after taking deep breaths in and blowing into a mouthpiece, and finally a tilt table test. The autonomic neurologist also took a medical history, list of symptoms, reviewed her medical records and previous testing, and performed a physical examination. His preliminary findings were that her sweat testing is abnormal and she has exercise intolerance, which means that her autonomic nervous system is not regulating itself as it should when she is exerting herself physically. For now, the doctor wrote a letter to her school stating her diagnosis and that her PE class needs to be adapted or modified to accommodate for her health needs. He will also be reviewing all her medical records in more detail over the next couple days, further analyzing the tests, and will write me with more complete recommendations.
E did a fantastic job at the testing and appointment and received many compliments about what a good patient she is. I could not be more proud of my brave girl! She definitely deserved a little fun after all that. So we headed to the theater to see the movie, Wonder. We were both anxiously awaiting the release of this movie after reading the book together earlier this year. It was such a touching movie (and book), and I really related to it on many levels, which left me tearing up throughout the movie. The message that sticks with me is the quote from J.M. Barrie that is referenced in Wonder...
However, today in this rare moment of quiet, I am able to think about all the things I am thankful for, and I think I need to do this more often. I want to consciously remind myself of all the ways we are blessed as a family, and I want to do this every month, not just in November. So here goes...
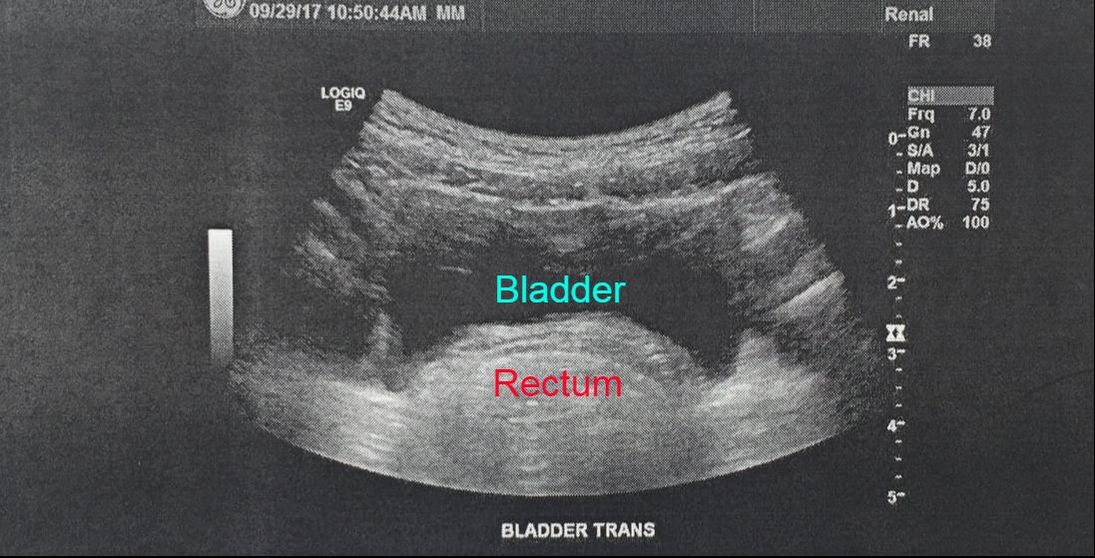
1. I am thankful for my husband, who stands by me and our daughters through all the ups and downs. I know he loves us all, and I am so, so grateful for him every day! 2. I am thankful for my three amazing daughters. They have taught me so much about love, patience, determination, and courage. Words will never express how much they mean to me! 3. I am thankful for my sisters, parents, aunts, uncles, cousins, and grandparents. They have all taught me so much during my life and many have been my rock and support system through all our challenges, tests, procedures and surgeries. I couldn't do it without them and love them so much. 4. I am thankful for the friends, that are like family, and have also been a tremendous support to me and my family. Ladies, I love you too! 5. I am thankful for the friends that I've met in online support groups. While some people don't see the value of Facebook, I do. It allows families, who have similar medical struggles and diagnoses, from all over the world to communicate and support each other. There is one special friend who has three children are similar to mine that I am very thankful for. I would be lost without her support! 6. I am thankful for each new day, that I have learned to keep advocating for my girls and never give up, for the medical team that we currently have that is fighting for my girls as hard as I am, and for all the progress we have made so far. 7. On that note, I am also thankful for the nurse practitioner who nominated our girls for Make A Wish Foundation. I received a voicemail message from Make A Wish Foundation yesterday. Fingers crossed that it's good news! I could go on and on, and I will. I plan to jot down reasons to be thankful each month. Despite the challenges, I know we have many blessings! Hopefully this Thanksgiving you are reminded of all the reasons you are thankful. Wishing you all a happy and blessed Thanksgiving! Thanks for reading! Sorry for the delay in writing updates! We've had a lot of appointments the past few weeks, and I've finally had a chance to sit down and write. I'll try to keep it is a brief as possible without leaving out important information. I also want to warn you that some of the updates involve information about constipation and how the digestive system works. Sorry if it makes any squeamish, but for those reading the blog looking for information related to their own health, those details are pertinent. So on October 2nd, the day finally arrived when one of our daughters had the opportunity to meet and be evaluated by the geneticist that specializes in Ehlers-Danlos Syndrome (EDS). Our oldest two daughters have been on the wait list to see him since March 2016, which puts us at 19 months of waiting. We were expecting to wait for 2 years and were so relieved when her GI motility specialist reached out to the geneticist and got her appointment scheduled so quickly. Yet, now that the day was finally here, I was a nervous wreck. So much has been hinging on this appointment, and so many of the girls' other doctors and specialists have been waiting for this evaluation too. As I was driving the 90 minutes to get to the appointment, all I could think of was how much I hoped he would provide help, answers, and confirmation that our 5-year-old daughter, A, also has Ehlers-Danlos Syndrome. So you can imagine my surprise when, after taking a full medical history on myself and all three of my daughters, the geneticist says, "Well, I wish I was comfortable saying that this was only EDS and that I could fully manage your family's care, but unfortunately I don't feel comfortable saying that at this time." He believes that there may be a bigger diagnosis that would encompass the constellation of symptoms and disorders that the 3 girls have. He's wondering if there is a neurological condition or possibly a mitochondrial disorder, as hypermobility can be caused by other syndromes and disorders. Yikes! That completely caught me off guard. I was expecting this appointment to be either a slam dunk, or like many other appointments, to be let down, dismissed or sent back to the drawing board. Sometimes, when doctors don't have the answers, they send you on your way without any direction or feedback. I've left those appointments feeling defeated, confused and in tears. So I was completely surprised when this appointment took a turn the other way, and he suggested that there is more going on medically that we originally thought. However, when discussing my medical history and symptoms, the geneticist said that it sounded like I have a typical case of EDS. How can that be, but the girls have more? On one hand, I was pleased that he was listening and validated our concerns. On the other hand, I was scared. The fear of the unknown is worse than the fear of the known, at least for me. Or as they say, "Better the devil you know, than the devil you don't know." I guess time will tell, and my questions will have to be answered in about 8 weeks time when we get the genetic test results. He said he would be happy to see our other girls if needed, but that we should wait until the results come back to determine the best treatment plan for our family. In other news, we had a few other appointments over past couple weeks. Our 8-year-old daughter, E, and our 4-year-old daughter, C, were at the hospital to have their clinic appointments with the GI, allergist and nutritionist on October 6th. It's nice to be able to have 6 appointments scheduled together and for the doctors to be able to collaborate. Yet, it also makes for a really long day, leaving the house at 8:00 am and returning by 2:30 pm. So the highlights from those appointments include that both girls continue to be constipated and in need of a bowel clean out. So for 3 days total that weekend, we completed clean outs for all 3 girls, which is never a pleasant experience and requires us to be home bound and missing out/cancelling a lot of activities. The GI added senna to C's medications for the next 2 weeks in hopes of keeping her digestive system moving. We also discussed with the GI and allergist how much C has been coughing, both when running or exerting herself and when drinking fluids. So the GI ordered a video flouroscopic swallow study to rule out aspiration when drinking and the allergist prescribed a rescue inhaler, Albuterol, to use as needed when she has trouble breathing and coughing when exercising or before exerting herself. Additionally, we were advised to stop the peanut butter trial for C for now, since it was causing abdominal pain. We will retest her food allergies in the winter when she is able to stop taking her antihistamines for 5 days prior to the skin allergy test. At that time, we hope to be able to trial foods that were previously triggers and that she is hopefully outgrowing. Then on October 11th, we had 2 important follow-up appointments with the motility specialist and the urologist. This was another very long day as we left the house at 8:45 am to drop off the girls at school, drove to the far north suburbs for the motility specialist appointment, got home around 3:00 pm, picked up the girls from the babysitter and school, had ABA therapy, ate a quick dinner, and then left for the urology appointment at 5:45 pm to get there in time for the 6:40 pm appointment. We didn't arrive back home until 8:00 pm. While these appointments are very important, the days are long and exhausting for all those involved. It also requires asking friends for help with getting kids to and from school, hiring a babysitter to pick up our preschooler and care for her, and for my husband to come home early from work to take over ABA therapy session, help them with homework, and finish the nightly routines before bedtime. I'm grateful for everyone's help, but wish our days weren't so complicated. I long for a simpler life... maybe someday. So first was the follow-up appointment with the motility specialist to go over the 3 motility tests that A, our 5-year-old, had done over the past month, which included the SITZ marker study, the water soluble contrast enema, and the Anorectal manometry test. The SITZ marker study showed that all the markers had been passed, but that there was still a lot of stool in her colon. Thankfully, the contrast enema test was also normal. So that means that her colon is not stretched out, which is surprising but also great news. Finally, the anorectal manometry test revealed that the muscle control in her rectum is abnormal and that she is contracting those muscles instead of relaxing them during an attempted bowel movement. This is likely due to her long history of severe constipation and pain. Her body has adapted to the pain and discomfort. So the recommended treatment is pelvic floor biofeedback therapy to address the pelvic floor dyssynergia. Furthermore, he increased her senna dosage and referred her to the multi-disciplinary bowel management program at the local children's hospital. This team includes the GI motility specialist, a pediatric surgeon, a social worker or psychologist and a nutritionist. That evening, our 4-year-old daughter, C, had her follow-up appointment with the urologist to review the results from the abdominal x-ray, abdominal ultrasound and the spinal MRI. Prior to this appointment, we had received a call from the neurosurgeon that the brain MRI showed a stable pineal cyst (see the post called My 12-hour adventure with "C" for more information), that the spinal MRI was normal, and no tethered spinal cord was noted. While this sounds like good news, it means further evaluation to identify why she's having current symptoms. However, the urologist did share this ultrasound photo with me, which shows C's bladder. He pointed out how her rectum is so full of stool that it is pushing into her bladder in an extreme way. He actually said to me that looking at that photo made him feel like he had to urinate (insert humor), but that in all seriousness, that it looks extremely uncomfortable. It was technically an obstruction and was blocking the elimination of stool and air in her entire colon. So that definitely explains why she has such severe abdominal pain on a weekly, sometimes daily, basis. He recommended that she continue the senna her GI prescribed for the next 3 months to keep her digestive system moving and cleaned out. Hopefully, the bladder symptoms will improve. We follow up with the urologist in 3 months, and she how she's doing. Thank you all for reading and for your support! Please feel free to leave comments or questions below, or contact me directly. It's always nice to hear from you!
Last Friday, September 29th, our 4-year-old daughter, C, underwent four different tests at the local children's hospital in Chicago. Boy, that was a long day! We left the house at 8:00 am to arrive for the abdominal ultrasound at 10:30 am with an abdominal x-ray immediately following that. Both of these tests were ordered by her urologist to check her anatomy and for any abnormalities that could be causing her urinary incontinence and urgency issues. I was reminded why these tests were necessary when we were only 5 minutes away from the hospital, and we had to make a pit stop at the Rock-n-Roll McDonald's because she had to use the restroom and couldn't wait. That gave me a chance to buy coffee and a breakfast sandwich since parking was free with a purchase. I ate breakfast quickly in the car without letting C know that I had food. She had to fast from midnight the night before due to the testing and wasn't happy about it. Luckily, the the first two tests were easy enough and were done quickly! She was a trooper and very cooperative (minus not liking the gel they use during the ultrasound). Next, she had the the full spinal and brain MRIs, which included being put under general anesthesia. The spinal MRI was the third test ordered by the urologist for her urinary incontinence, since this condition could be caused by having a tethered spinal cord. Her oldest sister, age 8, has had two surgeries already to repair her tethered spinal cord. So the urologist wants to rule that out as the possibility for C too. The brain MRI was to further evaluate the pineal cyst that we have been monitoring since she was 15 months old since she has a new onset of coughing and has speech delays that are not improving with speech therapy. (See my previous post on 9/17/17 for more info.) We had to check in at 2:00 pm, which meant we had 3+ hours to kill at the hospital. Thankfully, the cafeteria had orange jello and apple juice, which she could consume up until 12:30 pm since they were clear liquids. We also did a lot of walking around the hospital, visited the Sky Garden, played card games, visited the gift shop, bought the orange teddy bear, and took many trips up and down the escalator (her favorite part of the day!). The 2 MRIs went well. She tolerated the anesthesia just fine and woke up recovery a couple hours later. She was discharged by 6:00 pm; so we were right in time to sit in Friday evening rush hour (insert sarcasm). All in all, she was such a trooper during the 12-hour adventure! Now that we have that under our belt, we will hope and pray for answers and a direction towards treatment and management of her conditions. I'll be sure to keep you posted on the results and next steps. Thanks for reading and for all your prayers and support! It means a lot to our family.
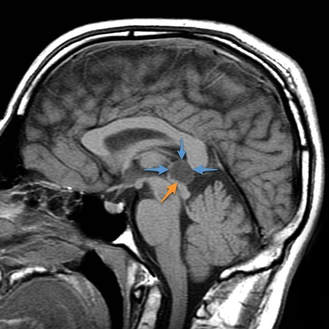
Last week, we was another busy week around here. There were 4 medical appointments, including a brain MRI, 8 therapy sessions, Curriculum Night at the elementary school for 2 of our kiddos, and a wheelchair delivery. So here's a recap of the important updates. Last Monday, our 4-year-old daughter, C, had a "quick", non-sedated brain MRI to check on her pineal cyst that was found in her very first MRI when she was 16 months old. A pineal cyst is a cyst that is found in the pineal gland, which is near the center of the brain in the cerebrum. The cerebrum's main function is to control thinking, learning, speech, emotions and movement. The pineal gland produces the hormone called melatonin, which helps regulate sleep cycles. (For more info, you can read more here.) The neurosurgeon had informed us 3 years ago that this cyst was benign and there was no reason to be concerned since pineal cysts are typically asymptomatic. However, he recommended that we should monitor it and repeat the brain MRI once per year to make sure it was not growing in size. So this past Monday was the 4th brain MRI she has had, and we were happy to hear that the cyst had not grown in size. When we discussed the results with the neurosurgeon, he had asked if she was having any headaches or other symptoms. I said no, but asked if her speech delays could be related. I explained that C has been in speech therapy since the beginning of June 2016 and has not made any progress after 15 months of therapy. While he never said it could be related, he did suggest immediately that she should have a 3 Tesla MRI, full brain scan. The 3 Tesla MRI shows the highest quality images. Since C is already scheduled for a full spinal MRI on September 29th, he wanted to add on the brain MRI and have them completed at the same time. We were always assured that there was no reason to worry about this benign cyst, and we therefore trusted what the doctor said and have not thought much about it from year to year. However, when I left the appointment this time, I decided to research what other symptoms are typical of children with symptomatic pineal cysts. Here's what I read from the National Institute of Health website. When a pineal cyst does cause symptoms, they may include headaches (the most common symptom), hydrocephalus, disturbances in vision, and Parinaud syndrome. Although rare, people with symptomatic pineal cysts may have other symptoms such as difficulty moving (ataxia), mental and emotional disturbances, vertigo, seizures, sleep (circadian rhythm) troubles, vomiting, hormonal imbalances that may cause precocious puberty, or secondary parkinsonism. This was quite alarming to me since C has struggled with sleep issues since she was 1, or possibly younger, and has been taking melatonin for several months to help her fall asleep at night. I'm thinking that it's not a coincidence that the cyst located in the pineal gland, which produces the hormone melatonin, is hindering her body's ability to make enough of melatonin on its own. She also has debilitating anxiety, symptoms that point to ADHD, and other "emotional disturbances." It also makes me wonder more about her speech delays since the location of the cyst is within the cerebrum which is the part of the brain that is responsible for speech. Needless to say, I am focused on finding more information and will definitely bring all these questions to her doctor(s) after we receive the results of her MRIs. In other news, the Convaid stroller/wheelchair, for our 8-year-old daughter, E, finally arrived on Wednesday after a 4-month wait. The representative quickly fitted her to be sure it was the correct size and gave me a crash course in how to use it. This device will come in handy when we go on family outings to the zoo, arboretum, and similar places, since E cannot usually walk for very long without fatigue, leg and ankle pain due to having Ehlers-Danlos Syndrome. We will now be able to have longer days away from home, she will be able to participate in activities that same age peers are doing, and it will give her the rest her body requires. She is very excited to have it and loves the color purple that she chose! Now, I just have to find a place to store this beast! While it is easy to push and use, it is quite bulky. As always, thanks for your continued support and for reading! Please sign up for our newsletter on the home page if you have not done so already.
Today, our 5-year-old daughter, "A", had outpatient surgery to patch a hole in her eardrum and to reduce the size of the turbinates in her nasal passage. We are hoping that the nasal surgery will improve her obstructive sleep apnea, which will be tested in sleep study in about 4-6 weeks. Needless to say, she was not excited about today's agenda and was very disappointed that she couldn't drink her "milk" this morning (which is actually a pediatric dairy-free supplemental formula). She didn't need to check in for the surgery until 10:00 am, and we were hoping she'd sleep in like she has been wanting to every school day. Well for those you that know us well, I'm sure you can predict that our wish did not come true. She was up by 6:30 am! So we had to distract her from wanting to drink her milk or eat breakfast for 3 hours. We thought she was handling the news of having her "ear fixed" pretty well, until it was time to leave. Her younger sister tried to console her, but eventually Dad had to just carry her out to the car, which broke my heart. During the car ride, Dad started playing the I Spy game. Thankfully, she calmed down and even had a bit of fun. After she got checked in and changed into her gown, they gave her some happy medicine to calm her nerves. She also got her polar bear and Skye from Paw Patrol ready for the procedure too! Thankfully, the procedure was complete in under an hour and Adam was able to join her in the recovery room. I'm happy to report that all went well and she is resting at home now. She'll be back to herself in no time!
In other news, I received a very exciting phone call this week. The geneticist's office, that specializes in Ehlers-Danlos Syndromes (EDS) that I mentioned in my first post, called this week to schedule A's evaluation with the geneticist and the physical therapist at his clinic! Our prayers were answered with the help of the motility specialist making the referral to the geneticist. She got bumped up on the wait list, and after 18 months, we finally have an appointment for her on October 2nd! I am so excited to finally meet this doctor after all I have heard and read about him. I feel like we are meeting a celebrity! Well, in the EDS world he kind of is a celebrity. He was actually awarded a Lifetime Achievement Award today at The Ehlers-Danlos Society Global Learning Conference taking place in Las Vegas this weekend. So October will hopefully yield long-awaited answers for A. We will also be meeting with the motility specialist on October 11th to review all of the motility testing results. Fingers crossed for a positive treatment plan moving forward! Please check back or subscribe to my newsletter to stay updated! If you are interested in learning more about the Ehlers-Danlos Syndromes, please visit the The Ehlers-Danlos Society's website. www.ehlers-danlos.com Many people are wondering where the name of the blog, Raising Zebras, came from and why the zebra is an animal that my family identifies with. I'm sorry to keep you waiting!
So why the zebra? It's not something I chose personally but something that I connected with after my oldest daughter and I were diagnosed with Ehlers-Danlos Syndrome (EDS) last year. The Ehlers-Danlos Society uses the zebra as their logo and they explain why in an article on their website [here]. I've taken this quote from their website: "People with the Ehlers-Danlos syndromes and hypermobile spectrum disorders (HSD) often identify themselves as zebras. Medical students have been taught for decades that, “When you hear hoofbeats behind you, don’t expect to see a zebra.” In other words, look for the more common and usual, not the surprising, diagnosis. But many of us spend years pursuing a diagnosis for disorders that aren’t well known. Or aren’t expected in someone who looks normal, or is too young to have so many problems, or too old. Or even, what we might have is considered too rare for anybody to be diagnosed with it. So the zebra became our symbol to mean, “Sometimes when you hear hoofbeats, it really is a zebra.” Ehlers-Danlos syndromes are unexpected because they’re rare." There are other rare diseases and syndromes that identify with the zebra for the same reason explained in the above quote. Our family has a few of these rare diseases/syndromes in addition to the Ehlers-Danlos Syndrome, such as Mast Cell Activation Syndrome, Dysutonomia/POTS, and Food Protein Induced Enterocolitis Syndrome (commonly referred to as FPIES). So the name of my blog was born from the fact that I am raising 3 daughters who have these rare diseases... my 3 amazing, brave zebras! Click on the links in blue for more information and please stay tuned for more! If you'd like to follow my blog and receive notifications of new posts by email, please visit the Home page and scroll down to the bottom to enter your email address in the form. Then click on "Sign Me Up" as seen in the image below. Thanks for reading! Well, as I launch my blog today, I know that there is a great deal of background that may be needed for those who don't know our family very well, and I will get to that soon. For today, I'm going to jump right in to our journey and tell you all about the wonderful experience we had with A's new motility specialist. (In the interest of privacy for our daughters, I will only refer to them by their first initial.) A, our middle daughter and currently 5 years old, was referred to this specialist because she has had chronic, severe constipation since she was an infant. She has seen a total of 3 GIs over the years, and is currently maxed out on the dosages of her 4 constipation medications, yet still deals with constipation. Her current GI has recommended that our next steps would either be to see a motility specialist for motility testing or to consider the MACE procedure.
So August 22nd, we went to the local children's hospital with A to meet "Dr. F", who is fairly new to the area. Previously, Chicago did not have a motility specialist and our oldest daughter, E, who is currently 8 years old, had to travel to Milwaukee in February 2016 for the same type of specialist and testing. So we were thrilled when our GI and urologist told us there was a new doctor here in Chicago. Luckily, our urologist is with the same children's hospital, made the referral, and got us an appointment in only 2 months (he is booking out appointments several months ahead typically). Great news, except E also had an appointment that same day at exactly the same time to have her G tube button changed out at our other favorite hospital across town. Neither appointment could be rescheduled without waiting 3-4 more months. So my husband took the day off from work and brought E to her G tube appointment. These complications in our schedule often arise, and I'm thankful that my husband is able to help like this occasionally. I'm also happy to report that E was amazingly brave with the G tube change... no tears and 3 more months to go before the next change! So back at the motility appointment with A, we met with Dr. F for about an hour in total. He took his time getting all the history and background, read through all the referral notes and medical records, and asked lots of questions. Dr. F was kind, compassionate, very knowledgeable, and had a wonderful bedside manner. He has experience with children on the autism spectrum and was understanding of the limitations we face daily. He assured me he wouldn't suggest anything that would not be practical for us and our daughter (i.e. no daily enemas! LOL!). When we got to the part of her medical history where I mentioned that I have Ehlers-Danlos Syndrome (EDS), that her doctors suspect that she may have it as well, and that we are on a 2-year waitlist to see the geneticist that specializes in EDS, he surprised me with the most wonderful news! He knows and works with this very same geneticist, and together they have treated many patients with EDS! I know the average person won't quite understand how amazing this actually is, but to put it in perspective, most doctors have not even heard of EDS. Yet this geneticist specializes in EDS, is a world-wide expert in this field, and was heading the committee that just published the new EDS diagnostic criteria and several research articles! So this was like hitting the jackpot for our family and an answer to my daily prayers! After Dr. F finished taking all the history, completing the physical examination, and determining her Beighton score for hypermobility, he was in agreement that further GI motility testing is needed, and that she should definitely see the geneticist sooner than later. Her Beighton Score was a 7 out of 9, which is a positive indicator for joint hypermobility, and one of the diagnostic criteria for Ehlers-Danlos Syndrome. So Dr. F wrote a personal referral note to the EDS geneticist and sent it while we were still at our appointment. He said that the two doctors will often do each other favors when referring patients to one another, and that it will hopefully get her an appointment sooner. Fingers crossed, as we have been on the waitlist since March of 2016! In the meantime, Dr. F ordered three motility tests for A: 1. SITZ marker study, while on medications 2. Water soluble contrast enema to assess colonic caliber 3. Anorectal manometry He will likely consider future colonic manometry testing, pending the results of the first three tests. Overall, we were very pleased with the outcome of the appointment and have hope again that we are on the right path to finding answers and a treatment plan. Stay tuned for updates on the testing! Thanks for reading and have a great day! |
AuthorHi, I'm Rebekah! I'm a wife, architect, teacher and mother to 3 amazing daughters! Thanks for stopping by my blog, RAISING ZEBRAS! Archives
February 2018
Categories |